There are 3 main ways we can increase Vitamin D in our blood and cells of our body:
- Expose our skin to sunlight.
- Eat foods with lots of Vitamin D.
- Take Vitamin D supplements.
Sunlight and UV-B Rays
The amount of Vitamin D that our skin can make after exposure to the sun varies enormously, depending on the following five factors:
- How much skin is exposed.
- The color of our skin. Darker skin needs more sun exposure than lighter skin, because the melanin pigment screens out the UV-B rays that promote Vitamin D synthesis [more info].
- The time of year. During the summer, the amount of light from the sun is much more intense than during the winter, and can stimulate Vitamin D synthesis more effectively.
- The latitude. The sun is more intense closer to the equator. Within North America, this means that the farther north we are, the less effective the sun is at stimulating Vitamin D synthesis.
- The time of day. Since the sun is more intense at high noon than it is in the morning or late afternoon, midday sun exposure will be more effective at stimulating Vitamin D synthesis.
All these variables make it impossible to recommend a specific amount of sun exposure. However, there are some general recommendations and findings to keep in mind:
- The darkest skin can have a 6-fold slower rate of Vitamin D synthesis than the palest skin, for a given amount of sunlight [1,2].
- During winter months, the skin of even white individuals living North of latitude 42˚ (Boston/Chicago/Omaha, NE/Medford, OR) is unlikely to be able to synthesize Vitamin D [3].
- Seasonal differences in UV-B intensity are much stronger at higher latitudes. For example, for a person with medium-color skin (Fitzpatrick III) exposing 25% of their skin to the sun at midday, to make 1000 U of Vitamin D, they would need 7 minutes in July, but 62 minutes in January (it’s generally not comfortable to expose 25% of one’s skin for an hour in the Boston winter!). In Miami, this seasonal difference is much smaller: the same person would need 6 minutes in July, and only 15 minutes in January [2].
- When seeking skin sun exposure, it is recommended that we expose not just our face, but also our arms and legs, and possibly even our torso. The reasons are that (i) there is much more skin area on these other body parts than our face, and so we can make more Vitamin D in a given amount of time; and (ii) our faces tend to have the most sun-damaged skin of our bodies, and so it is beneficial to rely on other body parts for sun exposure for Vitamin D.
- Exposure to the sun or other source of UV light, and its effect on any particular person’s skin, is often measured as the “Minimal Erythemal Dose”, or MED. This dose will depend on the variables above (skin color, time of year, latitude, etc), and is defined as the amount of sun that causes a very slight reddening of the skin that appears within 1-6 hours, and disappears within 24 hours. This is a mild effect that most of us would not even consider to be a sunburn. Importantly, the amount of amount of sun exposure needed to reach maximum Vitamin D synthesis in someone’s skin is just half this MED amount [4]! It was found that exposure of the arms and legs to half this MED amount is approximately equivalent to ingesting 3000 IU of Vitamin D [4,5].
- Sunscreen does somewhat reduce the amount of UV-B that will reaches the deep levels of our skin that make Vitamin D [6,7]. However, the calculations above and other findings suggest that if you are out in the summer sun, and use appropriate sunscreen to avoid burning, your skin will most likely have enough sunlight to make Vitamin D. On the other hand, during fall, winter, and spring, it may be advantageous to cut back on sunscreen.
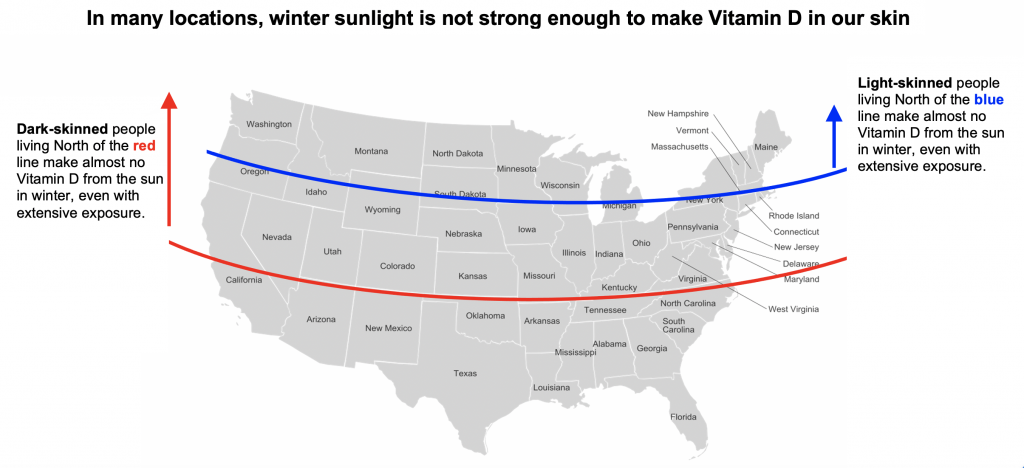
In many locations, winter sunlight is not strong enough to make Vitamin D in our skin
What About Skin Cancer Risk from the Sun?
The sun can both help us, by supporting Vitamin D synthesis, and hurt us, by causing sunburn and skin cancer. There is some controversy about whether people should even try to increase Vitamin D through the sun’s action on our skin, or whether the sun is too risky, and we should just take supplements to increase Vitamin D to meet our needs [7,8]. Others, however, argue that humans evolved to use the sun to make Vitamin D, and that the amount of sunshine needed to increase Vitamin D is much less than the amount of sun that causes us to burn and increases our risk of skin cancer [4,5]. Additionally, it has been shown that Vitamin D produced in the skin lasts longer in our bodies than Vitamin D taken as a supplement [4,9]. Moreover, Vitamin D also has potent anti-cancer effects on its own [10-12].
In summary, for most people, it probably makes sense to get some direct sun on our skin throughout the year. Pale-skinned people should be careful in the summer to avoid getting so much sun at one time, or on a few highly exposed areas (eg face) that they burn, whereas darker-skinned people generally have a lower risk of skin damage by the sun, and a greater need for Vitamin D.
Vitamin D in Foods
Some foods are naturally rich in Vitamin D, whereas others are commonly supplemented with Vitamin D.
Dairy foods including milk and yogurt are often fortified in the US, where an 8-oz glass of enriched milk typically has 100-150 IU of Vitamin D [13,14]. Other fortified foods can include orange juice, tofu, cheese, breakfast cereals and infant formula (also about 100 IU/serving; [14]). Nutrition labels will tell you whether a food has Vitamin D and how much.
Foods that naturally contain Vitamin D include fatty fish (eg. wild salmon, herring, 300-1000 IU/3.5oz serving; more if their livers are consumed), eggs (20 IU/yolk), and some mushrooms [4,15]. Remarkably, the Vitamin D content of mushrooms can be increased dramatically by drying them in the sun [4,16]. In general, aside from fatty fish livers and sun-dried mushrooms, it is difficult to naturally obtain our Vitamin D needs through diet alone.
Vitamin D Supplements
For most people, taking Vitamin D supplements will be the easiest way to increase Vitamin D in the blood up to desired levels. Vitamin D supplements are available as D2 (ergocalciferol) and D3 (cholecalciferol), with D3 generally thought to be slightly more effective [17]. Supplements are available without a prescription at 400 IU – 5000 IU per capsule. Prescription-strength Vitamin D is generally 50,000 IU/capsule, and injections of Vitamin D up to 200,000 IU may be given to severely Vitamin D-deficient individuals to increase Vitamin D. Keep in mind that since Vitamin D is fat-soluble, most of the supplements come in oil capsules, and the best time to take supplements is with your biggest meal of the day [18].
Cod liver oil is not highly recommended for Vitamin D supplementation because levels of Vitamin D can be low, depending on extraction process, and because cod liver oil also contains high levels of Vitamin A that can become toxic if large amounts are ingested [19].
How Long Does Vitamin D Last in Our Bodies?
As a fat-soluble nutrient, Vitamin D gets stored in our tissues, and so we don’t need to worry about variations day-to-day. In fact, Vitamin D levels in our bodies appear to decline slowly over a period of months after either normal summer exposures to sunshine, or a huge dose in a clinical trial [20,21].
REFERENCES
Clemens, T. et. al. 1982. Increased skin pigment reduces the capacity of skin to synthesise vitamin D3. Lancet 1:74.
Terushkin, V. et. al. 2010. Estimated equivalency of vitamin D production from natural sun exposure versus oral vitamin D supplementation across seasons at two US latitudes. J. Amer. Acad. Dermatol. 62:929.
Webb, A. et. al.. 1988. Influence of season and latitude on the cutaneous synthesis of vitamin D; exposure to winter sunlight in Boston and Edmonton will not promote vitamin D3 synthesis in human skin. J. Clin. Endocrin. Metab. 67: 373.
Holick, M. et al. 2011. Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline. J. Clin. Endocrinol. Metab. 96:1911.
Webb, A. and Engelsen, O. 2020. Ultraviolet Exposure Scenarios: Balancing Risks of Erythema and Benefits of Cutaneous Vitamin D Synthesis. Adv. Exp. Med. Biol. 1268:387.
Matsuoka, L. et al. 1987. Sunscreens suppress cutaneous vitamin D3 synthesis. J. Clin. Endocrinol. Metab. 64:1165.
Passeron, T. et al. 2019. Sunscreen photoprotection and vitamin D status. Br. J. Dermatol. 181:931.
Moan, J. et. al. 2008. Addressing the health benefits and risks, involving vitamin D or skin cancer, of increased sun exposure. Proc. Natl. Acad. Sci. USA. 105:668.
Haddad, J. et al. 1993. Human plasma transport of vitamin D after its endogenous synthesis. J. Clin. Invest. 91:2552.
Lappe, J. et. al. 2007. Vitamin D and calcium supplementation reduces cancer risk: results of a randomized trial. Am. J. Clin. Nutr. 85:1586.
Maalmi, H. et al. 2014. Serum 25-hydroxyvitamin D levels and survival in colorectal and breast cancer patients: systematic review and meta-analysis of prospective cohort studies. Eur. J. Cancer. 50:1510.
Holick, M. et al. 2014. Cancer, sunlight and vitamin D. J. Clin. Transl. Endocrinol. 1:179.
National Institutes of Health Office of Dietary Supplements. Vitamin D Fact Sheet for Consumers
Miller, G. 2019. Ask Dr. Dairy: How Much Vitamin D is in Milk? National Dairy Council Undeniably Dairy.
The Nutrition Source: Vitamin D. Harvard Chan School of Public Health.
Urbain, P. et al. 2011. Bioavailability of vitamin D2 from UV-B-irradiated button mushrooms in healthy adults deficient in serum 25-hydroxyvitamin D: a randomized controlled trial. Eur. J. Clin. Nutr. 65:965.
Tripkovic, L. et al. 2012. Comparison of vitamin D2 and vitamin D3 supplementation in raising serum 25-hydroxyvitamin D status: a systematic review and meta-analysis. Am. J. Clin. Nutr. 95:1357
Mulligan, G. and Licata, A. 2010. Taking vitamin D with the largest meal improves absorption and results in higher serum levels of 25-hydroxyvitamin D. J. Bone Miner. Res. 25:928.
Cannell, J. et. al. 2008. Cod Liver Oil, Vitamin A Toxicity, Frequent Respiratory Infections, and the Vitamin D Deficiency Epidemic. Ann. Otol. Rhinol. Laryngol. 117:864.
Ilahi, M. et. al. 2008. Pharmacokinetics of a single, large dose of cholecalciferol. Am. J. Clin. Nutr. 87:688.
Kroll, M. et. al. 2015. Temporal relationship between vitamin D status and parathyroid hormone in the United States. PLoS One. 10: e0118108.